登录方式
方式一:
PC端网页:www.rccrc.cn
输入账号密码登录,可将此网址收藏并保存密码方便下次登录
方式二:
手机端网页:www.rccrc.cn
输入账号密码登录,可将此网址添加至手机桌面并保存密码方便下次登录
方式三:
【重症肺言】微信公众号
输入账号密码登录
注:账号具有唯一性,即同一个账号不能在两个地方同时登录。
作者:段均
低氧性呼吸衰竭的呼吸力学评价
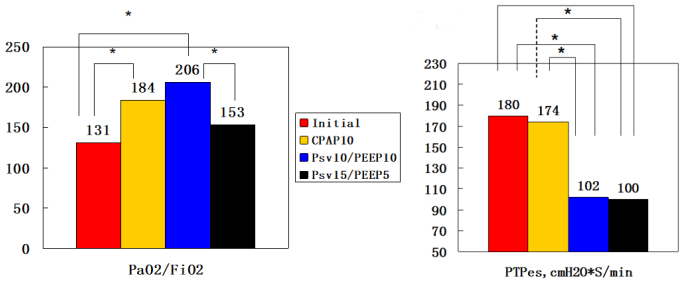
无创通气(NIV)生理效应
NIV能够降低低氧性呼吸衰竭患者的跨膈压和食道压,减少呼吸做功,改善氧合,降低PaCO2[2]。
综上,对于氧合指数200~300 mmHg低氧性呼吸衰竭患者,早期NIV可能降低插管率,肺外ARDS可能获益更多,但仍需大样本研究证实。
经鼻高流量氧疗(HFNC)生理效应
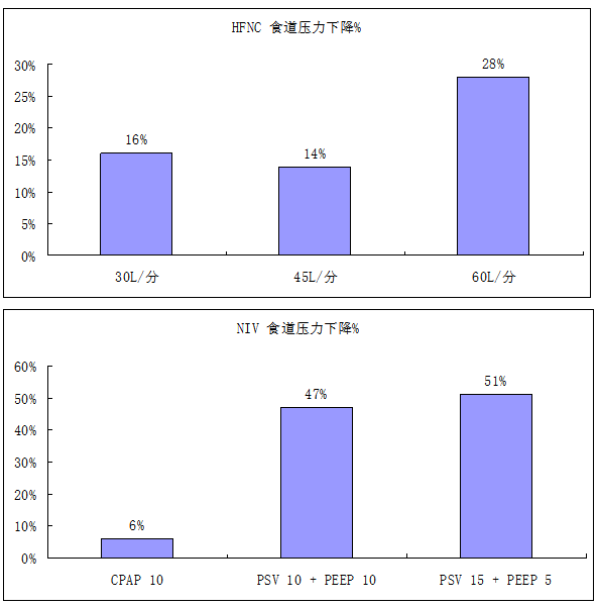
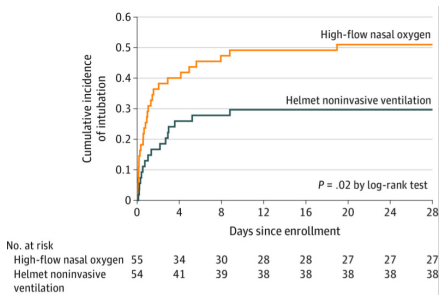
结合上述研究结果,我们得出结论:①头罩NIV优于面罩NIV,本质是头罩能给予较高的PEEP。如果面罩NIV也能给予较高的PEEP,是否会与头罩NIV等效?②面罩NIV+HFNC优于HFNC,本质是NIV的效应优于HFNC。患者能持续24 h耐受NIV,是否优于间断使用?
NIV在肺内源性ARDS和肺外源性ARDS患者中的应用
小结
参考文献
[1] L'Her E, Deye N, Lellouche F, et al. Physiologic effects of noninvasive ventilation during acute lung injury[J]. Am J Respir Crit Care Med, 2005, 172(9):1112-1118.
[2] Kallet R H, Diaz J V. The physiologic effects of noninvasive ventilation[J]. Respir Care, 2009, 54(1):102-115.
[3] Ferrer M, Esquinas A, Leon M, et al. Noninvasive ventilation in severe hypoxemic respiratory failure: a randomized clinical trial[J]. Am J Respir Crit Care Med, 2003, 168(12):1438-1444.
[4] Zhan Q, Sun B, Liang L, et al. Early use of noninvasive positive pressure ventilation for acute lung injury: a multicenter randomized controlled trial[J]. Crit Care Med, 2012, 40(2):455-460.
[5] Luo J, Wang M Y, Zhu H, et al. Can non-invasive positive pressure ventilation prevent endotracheal intubation in acute lung injury/acute respiratory distress syndrome?A meta-analysis[J]. Respirology, 2014, 19:1149-1157.
[6] He H, Sun B, Liang L, et al. A multicenter RCT of noninvasive ventilation in pneumonia-induced early mild acute respiratory distress syndrome[J]. Crit Care, 2019, 23:300
[7] Möller W, Celik G, Feng S, et al. Nasal high flow clears anatomical dead space in upper airway models[J]. J Appl Physiol (1985), 2015, 118(12):1525-1532.
[8] Delorme M, Bouchard P A, Simon M, et al. Effects of High-Flow Nasal Cannula on the Work of Breathing in Patients Recovering From Acute Respiratory Failure[J]. Crit Care Med, 2017, 45(12):1981-1988.
[9] Xuan L, Ma J, Tao J, et al. Comparative study of high flow nasal catheter device and noninvasive positive pressure ventilation for sequential treatment in sepsis patients after weaning from mechanical ventilation in intensive care unit[J]. Ann Palliat Med, 2021, 10(6):6270-6278.
[10] Mauri T, Alban L, Turrini C, et al. Optimum support by high-flow nasal cannula in acute hypoxemic respiratory failure: effects of increasing flow rate[J]. Intensive Care Med, 2017, 43(10):1453-1463.
[11] L'Her E, Deye N, Lellouche F, et al. Physiologic effects of noninvasive ventilation during acute lung injury[J]. Am J Respir Crit Care Med, 2005, 172(9):1112-1118.
[12] Zhao H, Wang H, Sun F, et al. High-flow nasal cannula oxygen therapy is superior to conventional oxygen therapy but not to noninvasive mechanical ventilation on intubation rate: a systematic review and meta-analysis[J]. Crit Care, 2017, 21(1):184.
[13] Frat J P, Thille A W, Mercat A, et al. High-flow oxygen through nasal cannula in acute hypoxemic respiratory failure[J]. N Engl J Med, 2015, 372:2185-2196.
[14] Frat J P, Brugiere B, Ragot S, et al. Sequential application of oxygen therapy via high-flow nasal cannula and noninvasive ventilation in acute respiratory failure: an observational pilot study[J]. Respir Care, 2015, 60(2):170-178.
[15] Thille A W, Muller G, Gacouin A, et al. Effect of Postextubation High-Flow Nasal Oxygen With Noninvasive Ventilation vs High-Flow Nasal Oxygen Alone on Reintubation Among Patients at High Risk of Extubation Failure: A Randomized Clinical Trial[J]. JAMA, 2019, 322:1465-1475.
[16] Grieco D L, Maggiore S M, Roca O, et al. Non-invasive ventilatory support and high-flow nasal oxygen as first-line treatment of acute hypoxemic respiratory failure and ARDS[J]. Intensive Care Med, 2021, 47(8):851-866.
[17] Grieco D L, Menga L S, Raggi V, et al. Physiological Comparison of High-Flow Nasal Cannula and Helmet Noninvasive Ventilation in Acute Hypoxemic Respiratory Failure[J]. Am J Respir Crit Care Med, 2020, 201(3):303-312.
[18] Patel B K, Wolfe K S, Pohlman A S, et al. Effect of Noninvasive Ventilation Delivered by Helmet vs Face Mask on the Rate of Endotracheal Intubation in Patients With Acute Respiratory Distress Syndrome: A Randomized Clinical Trial[J]. JAMA, 2016, 315(22):2435-2441.
[19] Grieco D L, Menga L S, Cesarano M, et al. Effect of Helmet Noninvasive Ventilation vs High-Flow Nasal Oxygen on Days Free of Respiratory Support in Patients With COVID-19 and Moderate to Severe Hypoxemic Respiratory Failure: The HENIVOT Randomized Clinical Trial[J]. JAMA, 2021, 325(17):1731-1743.
[20] Shu W, Guo S, Yang F, et al. Association between ARDS Etiology and Risk of Noninvasive Ventilation Failure[J]. Ann Am Thorac Soc, 2022, 19(2):255-263.
[21] Bai L, Ding F, Xiong W, et al. Early assessment of the efficacy of noninvasive ventilation tested by HACOR score to avoid delayed intubation in patients with moderate to severe ARDS[J]. Ther Adv Respir Dis, 2022 Jan-Dec;16:17534666221081042.
[22] Duan J, Han X, Bai L, et al. Assessment of heart rate, acidosis, consciousness, oxygenation, and respiratory rate to predict noninvasive ventilation failure in hypoxemic patients[J]. Intensive Care Med, 2017, 43(2):192-199.
[23] Bai L, Ding F, Xiong W, et al. Early assessment of the efficacy of noninvasive ventilation tested by HACOR score to avoid delayed intubation in patients with moderate to severe ARDS[J]. Ther Adv Respir Dis, 2022, 16:17534666221081042
作者简介
重庆医科大学附属第一医院呼吸与危重症医学科 副主任呼吸治疗师
中国医师协会呼吸医师分会委员
中国医学装备协会呼吸病学装备专委会委员
重庆市康复医学会呼吸康复专委会常务委员
Frontiers in Medicine客座主编,Canadian Respiratory Journal客座编辑,Thorax(中文版)编委
研发无创通气有效性评价量表、联合首创有创-无创双模式闭环通气撤机等技术,获中华医学会呼吸病学分会高影响力呼吸学术论文奖
 后可发表评论
后可发表评论




友情链接
联系我们
 公众号
公众号
 客服微信
客服微信